
Feet First
Wear the correct footwear and you'll avoid many injury problems, however some of us just have difficult feet that need lots of attention. We asked podiatrist Emma Lincoln for advice
Athlete's Foot
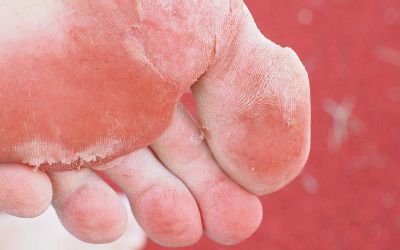
A fungal skin infection of which symptoms include itching and/or burning in-between the toes and soles of the feet. Skin can become red and flaky.
The condition is easily treated with an anti-fungal spray applied between the toes and soles. It is vital to persist with treatment for 1-2 weeks after symptoms have resolved in order to prevent recurrent infections. Wiping tea tree oil over the infected areas is effective in addition to the medicated anti-fungal spray as it has great anti-fungal properties.
The fungus thrives in hot, sweaty and moist feet so alongside these topical treatments good foot hygiene is essential. Wash and dry feet well (especially in-between the toes), change socks and vary footwear often and wash trainers and insoles regularly. Anti-fungal spray should be used in footwear. If untreated, the fungal infection can spread to the toenails, a condition called Onychomycosis.
Blisters
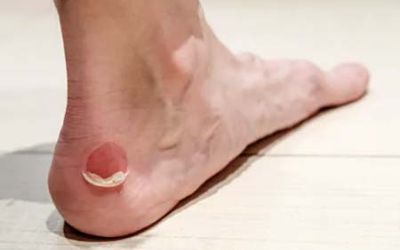
Caused by friction due to continuous rubbing from socks and footwear. This repetitive micro-trauma causes the layers of the skin to separate and fill with fluid. If deeper layers of the skin are damaged a blood blister will form.
In order to avoid this problem, wear in new running trainers gradually and never run long distances or races in trainers that still need 'breaking in'. Invest in running socks that help to remove excess moisture away from the feet. Applying Vaseline on problematic areas before a run will help to reduce friction and silicone plasters such as Compeeds are great for tender areas as they are thicker and more durable than ordinary plasters or strapping. When running, try to keep feet and trainers as dry as possible as blisters will develop quicker in wet feet, socks or shoes.
How do you know when to pop a blister?
There are both pros and cons to popping blisters. If the blister is small and not painful it is usually best to leave it. However, large blisters on weight-bearing areas or the heel tend to be more problematic. If the edge of the blister is red and inflamed or the colour of the fluid changes, it is advisable to pop the blister. It is important to be aware that bursting will leave an open wound that could potentially become infected. When draining a blister always use a sterile needle, don't remove the over-lying skin and cover with an anti-septic dressing for a few days.
Ingrown toenails

An ingrown toenail is caused by the nail growing into and piercing the side of the skin, resulting in tenderness and localised inflammation. They can arise due to the shape of the nail, trauma, poor nail cutting by either cutting the nail too short or cutting down the edges of the nail and inappropriate or narrow footwear.
Mild ingrown toenails can usually be managed with conservative treatment, however if the problem is persistent or the ingrown toenail becomes infected, nail surgery is required to permanently resolve the problem.
Achilles tendonitis
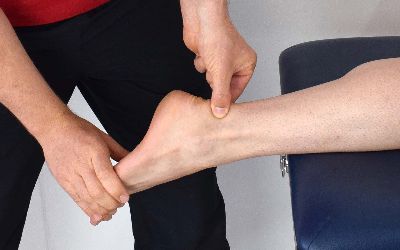
Inflammation of the Achilles tendon. Symptoms include pain in the tendon during and post exercise, swelling over the Achilles, pain on palpation and aggravation of the problem in flat shoes. It is often an overuse injury, however pronation and general poor biomechanics also contribute. Episodes of trauma, tight calf muscles, inappropriate or worn footwear and repetitive high impact activities on hard surfaces can also trigger the problem. The severity of the condition can range from inflammation of the tendon and sheath and small tears in the tendon to partial ruptures.
Initial treatment involves rest, ice, compression and elevation alongside anti-inflammatory medication and gels. Seek treatment from a podiatrist to address the biomechanics of the foot with the help of strapping, heel raises to take the Achilles off stretch, insoles or orthotics. Avoid any uphill running as this places extra stress and stretch on the Achilles.
It is vital to address tendonitis early to ensure a full recovery. In the acute stages, be patient, don't return to activity or running too soon as this will aggravate the condition and delay recovery.
Shin splints

One of the most common running injuries results in pain and tenderness predominantly in the lower third of the shin. It is caused by a stress reaction to the lining of the bone on the inner side of the tibia, where the tibialis posterior muscle attaches. Pain is usually worse during or post activity and can persist to the following day. It can be caused by over-training, increasing running distance or intensity, poor biomechanics, training on hard surfaces and inadequate or old trainers.
Treatment involves addressing the biomechanics of the foot and correcting excessive pronation. Investing in decent running trainers suited to your foot type is key. As regular readers will be aware, many running shops now have gait plates, which distinguish your foot type, helping to select the best trainer. Rest, alongside regular icing is essential in the early stages of a flare up to reduce acute inflammation. Avoid running downhill and regularly stretch out all muscle groups. During a rest period, non-weightbearing exercise such as cycling or swimming will help to maintain fitness levels.
Plantar Fasciitis

This is one of the most common causes of heel pain, triggered by the inflammation of the plantar fascia. The plantar fascia is a thick fibrous band of tissue originating at the heel bone that runs down towards the forefoot. Symptoms include pain under the heel, typically the inside of the heel where the fascia attaches to the bone. Pain is palpable and there is usually a central area of tenderness. Pain is worse first thing in the morning upon weight-bearing as the fascia tightens overnight and the discomfort tends to subside after walking for a short while. Symptoms can also return at the end of the day or after periods of increased activity or walking. Tight calf muscles, being over weight and having flat feet are the main culprits as pronation causes extra stretching and strain on the fascia.
Treatment includes rest, strapping and ice therapy with a frozen orange or round water bottle that can be rolled up and down the arch and massaged under the heel. Anti-pronatory insoles are essential, alongside anti-inflammatory medication and stretching of the planar fascia, Achilles and calf muscles. In more chronic cases, steroid injections can be effective.







